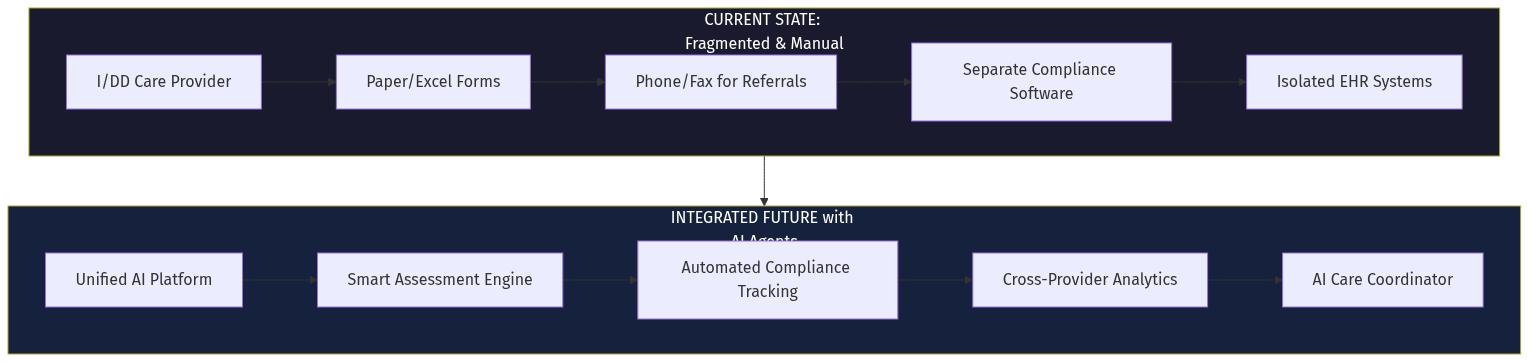
The Intellectual and Developmental Disabilities (I/DD) care sector represents a $70 billion annual market in the US alone — fragmented across 48 states with incompatible regulations, manual workflows, and zero interoperability. Kibu, a revenue-generating startup, proves the market is workable. But the real opportunity isn't incremental improvement. It's full-stack AI agents that can:
- Assess clients automatically using conversational AI
- Monitor compliance in real-time across state lines
- Coordinate care across 100+ provider organizations
- Transact billing and referrals autonomously