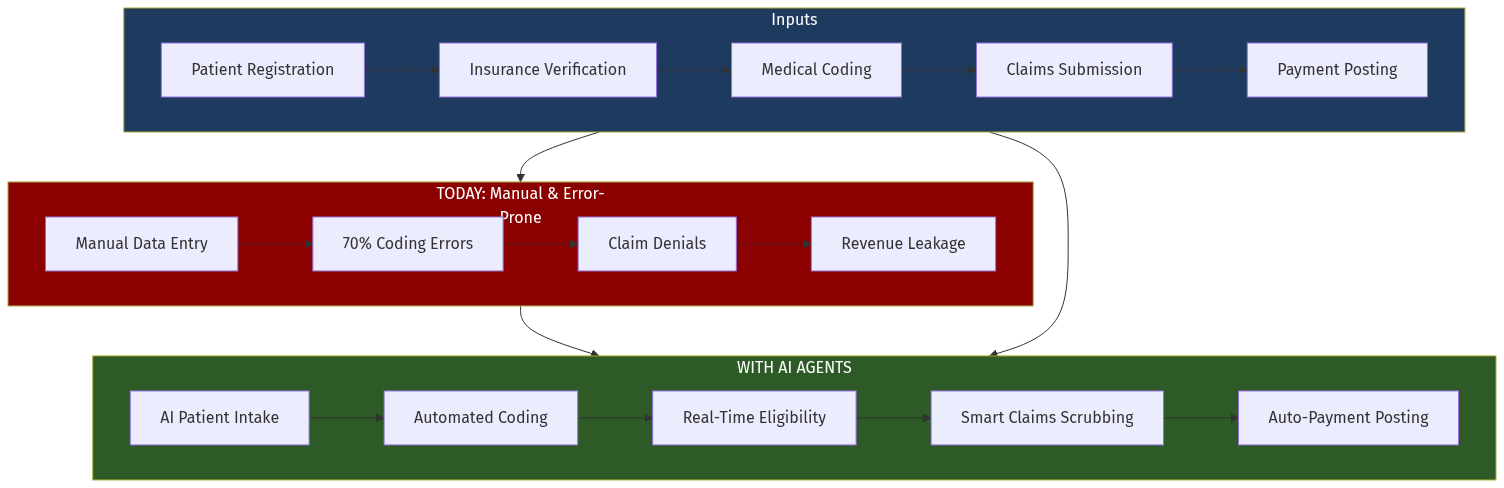
Healthcare Revenue Cycle Management (RCM) is the backbone of every hospital, clinic, and diagnostic center. It spans patient registration, insurance verification, medical coding, claims submission, payment posting, and denial management. In the US, RCM is a $150B industry with established players like Change Healthcare, Avaya, and Waystar.
India's healthcare RCM market is worth $45B—and it's broken.
Mid-market hospitals (200-2000 beds) lose 4-8% of revenue to claim denials. Small nursing homes and clinics struggle with insurance paperwork that consumes 30-50% of staff time. The few "automation" solutions that exist are legacy enterprise systems requiring 6-month implementations and crores in licensing fees.
This is the perfect conditions for an AI-native RCM platform:
- Massive leakage: 4-8% of all claims denied or underpaid
- Fragmented supply: No dominant player in the mid-market segment
- WhatsApp-native users: Indian healthcare staff live on WhatsApp—any solution must meet them there
- Regulatory complexity: Every insurance provider, every state, every procedure has different requirements
- Talent scarcity: Skilled medical coders and billing staff are in short supply