Anomaly Hunting: What's Strange About This Market
Anomaly 1: Policybazaar is a $1B+ company but has never been profitable. Why? Customer acquisition cost exceeds lifetime value. The missing piece: ongoing engagement (renewals, cross-sell) that creates LTV > CAC.
Anomaly 2: Acko and Digit raised $500M+ combined and still only have ~5% market share. The reason: building own products limits distribution. A marketplace model with AI on top would win.
Anomaly 3: 5 million agents exist but 70% are inactive. The reason: they can't earn enough from the administrative work. AI that handles admin lets them focus on selling.
Gap 1: The "Amazon for Insurance" That Actually Completes Transactions
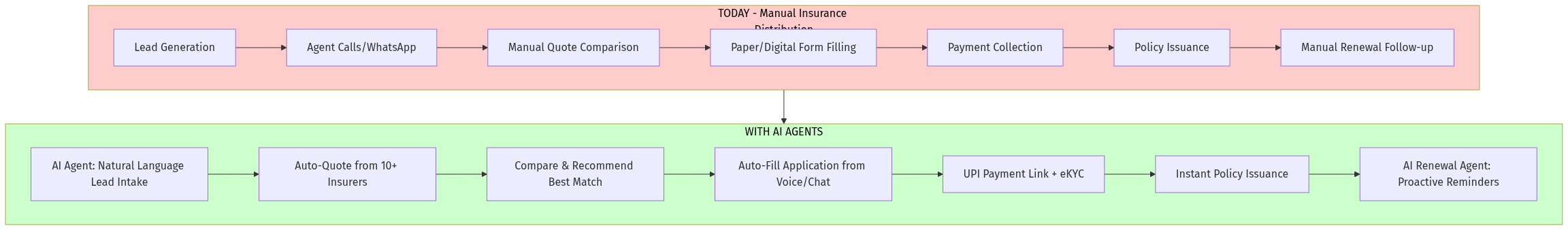
Current portals are lead generators. The AI agent:
- Captures intent via WhatsApp/voice
- Queries all insurers in parallel
- Auto-completes the application using Aadhaar eKYC
- Issues policy in 15 minutes (for simple products)
- Manages renewals proactively
Gap 2: The "Uber for Insurance Agents"
AI co-pilot for agents:
- Listen to customer call, auto-populate form
- Show real-time quote comparison
- Push best recommendation
- Auto-send follow-up messages
- Agent productivity 10x, commission stays same
Gap 3: B2B Group Insurance Marketplace
SME group health is a $5B+ market with:
- No comparison shopping (employers don't know what others pay)
- Renewal blindness (80% auto-renew without negotiation)
- Claims data opacity (employers don't know insurer performance)
AI platform: compares group quotes, tracks claims ratios, auto-renegotiates at renewal.
Gap 4: AI Claims Assistant
60% of claim rejections are due to documentation. AI agent:
- Reads the claim form
- Tells customer what's missing before submission
- Flags red flags (pre-existing conditions not declared)
- Tracks claim status, nudges for updates
- Result: 40% faster processing, higher satisfaction