The US healthcare system serves over 8 million individuals with intellectual and developmental disabilities (I/DD). These individuals receive care from over 60,000 provider organizations across 48 states. Every single one of these organizations must comply with state-level regulations, maintain meticulous documentation, and submit regular reports to state agencies.
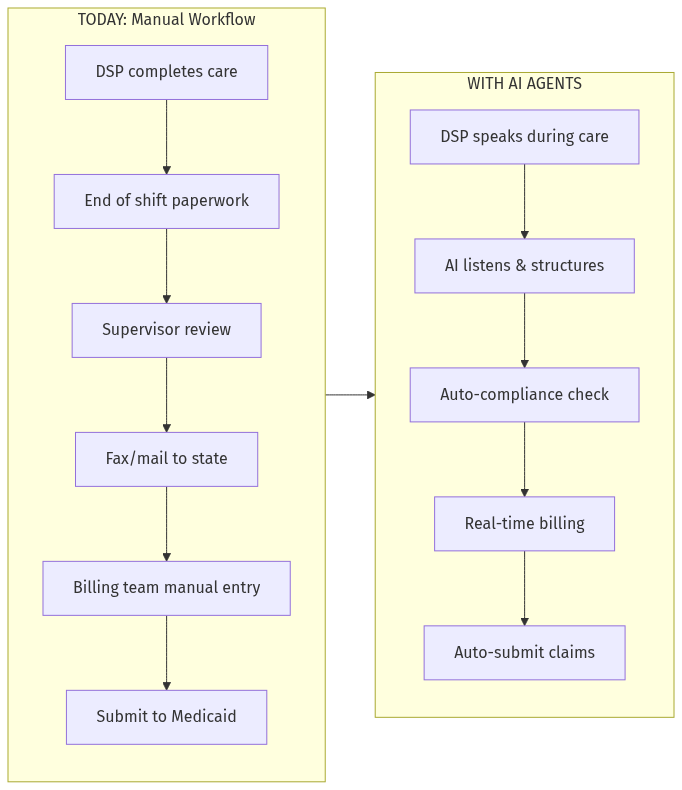
Kibu — currently generating $234K/month — has digitized one corner of this market. But the market remains 90% fragmented, manual, and desperate for AI agents.
This is a textbook vertical SaaS opportunity: high compliance friction, fragmented suppliers, repeat purchase behavior, and massive whitespace for AI-native reconstruction.